Similar migration for medial congruent and cruciate-retaining tibial components in an anatomic TKA system: a randomized controlled trial of 60 patients followed with RSA for 2 years
Albin CHRISTENSSON, Magnus TVEIT, Uldis KESTERIS, and Gunnar FLIVIK
Department of Orthopedics, Skåne University Hospital, Clinical Sciences, Lund University, Lund, Sweden
Background and purpose — There is an ongoing debate regarding the appropriate level of constraint in primary TKA. To provide increased stability and better kinematics, more resembling a natural knee, a medial congruent (MC) tibial insert has been introduced. To investigate potential impact on implant migration, we evaluated the cemented Persona TKA, randomizing between MC and cruciate-retaining (CR) tibial designs.
Patients and methods — 60 patients with primary osteoarthritis were randomized to either the CR or MC tibial component. Radiostereometric analysis (RSA) examinations, evaluating translational and rotational migration as well as maximal total point motion (MTPM), were performed on the first postoperative day, at 3 months, and 1 and 2 years after surgery. Preoperative, and 1- and 2-year patient-reported outcome measures (PROMs) data (KOOS and FJS) were collected.
Results — The mean tibial MTPM at 3 months were 0.48 mm (95% CI 0.37–0.58) and 0.56 mm (0.45–0.67) for the CR and MC respectively. 2 years postoperatively the respective values were 0.62 mm (0.50–0.73) and 0.73 mm (0.49–0.96). There was no statistically significant difference in migration between groups, for either the femoral or the tibial component, regarding x-, y-, and z-translations or rotations.
Both CR and MC groups improved as expected in PROM scores pre- to postoperatively, but without a statistically significant difference between groups. There were no revisions or other serious adverse events related to surgery.
Interpretation — The results are promising, indicating good fixation for both designs, and this is in line with other well-performing TKAs on the market. The increased medial congruity of the MC inlay does not seem to affect the migration or the PROMs up to 2 years.
Citation: Acta Orthopaedica 2022; 93: 68–74. DOI http://dx.doi.org/10.1080/17453674.2021.1983709.
Copyright: © 2021 The Author(s). This is an Open Access article distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (https://creativecommons.org/licenses/by-nc/4.0/), allowing third parties to copy and redistribute the material in any medium or format and to remix, transform, and build upon the material for non-commercial purposes, provided proper attribution to the original work.
Submitted: 2021-03-28. Accepted: 2021-09-01. Published: 2022-01-03.
Correspondence: albin.christensson@med.lu.se
AC: Compiled, analyzed, and organized the data, and wrote the manuscript. MT, UK, and GF: Study design. Performing operations. Actively participated in the research, revision of the manuscript, and approved the article for submission.
The authors wish to thank Håkan Leijon at the RSA laboratory, Skåne University Hospital, for help in computerizing the RSA images, and research secretary Åsa Björkqvist, Department of Orthopedics, Skåne University Hospital, for keeping track of all the patients. Also, thanks are offered to Helene Jacobsson, Statistician, Clinical Studies Sweden—Forum South, Skåne University Hospital, for statistical advice.
Acta thanks Geir Hallan and Arne Lundberg for help with peer review of this study.
The design of knee implants for total knee arthroplasty (TKA) has undergone many modifications in order to replicate the normal anatomy and function of the knee. However, despite great advancements, a significant number of patients are still dissatisfied with the result (Bourne et al. 2010).
For many years, the role of the posterior cruciate ligament and level of constraint of the polyethylene insert has been under debate, and scientific evidence for choosing one over the other is limited (Kärrholm and Saari 2005). To better reproduce the functional anatomy and replicate tibiofemoral kinematics, while still retaining the cruciate ligament, the medial congruent (MC) tibial design has been introduced to the market. The geometry of the MC components is designed to add stability to the medial compartment while enabling the lateral condyle to roll back in flexion (Blaha 2004), better resembling the motion of a normal knee. So far, studies have shown comparable survivorship of the MC compared with the traditional TKA designs (Cassar-Gheiti et al. 2020), and 1 study trended towards better PROM results for those receiving MC compared with cruciate-retaining (CR) components (French et al. 2020).
The Persona TKA (Zimmer Biomet, Warsaw, IN, USA) was introduced in 2012 and claimed to be a more personalized knee system. Compared with its precursor, NexGen, it comes with side-specific tibial components, together with more implant sizes and insert heights. A new feature is also the option of the MC tibial insert.
When new implants and designs are introduced, it is advisable to do this as a staged introduction, which includes studies on migration behavior (Malchau et al. 2011). Radiostereometric analysis (RSA) is a method of quantifying the 3D migration between implant and host bone over time (Valstar et al. 2005) and has been shown to predict late mechanical loosening (Kärrholm et al. 1994, Ryd et al. 1995, Pijls et al. 2012).
A different degree of constraint might affect the load and consequently migration pattern of the components. Therefore, the primary goal of this randomized controlled study was to compare the 3D micromotion, as measured with RSA, of the cemented CR and MC tibial components as well as for the femoral component in the Persona TKA. A secondary goal was to evaluate any difference in patient-reported outcome measures (PROMs) between groups
Patients and methods
The study was designed as a single-blinded, prospective trial. 60 patients, mean age 66 years (SD 9), with primary knee osteoarthritis and scheduled for TKA at Skåne University Hospital, Sweden, were included in the study (Tables 1 and 2). All procedures were performed from September 2017 to August 2018 by 3 experienced arthroplasty surgeons (GF, MT, and UK), trained in the Persona TKA system and who had performed at least 10 cases each before the start of the study. The patients were randomized in blocks to receive either a conventional CR or a MC tibial insert, so each surgeon should do 10 of each design. The randomization forms were prepared according to software randomization and put into numbered closed envelopes, opened at surgery after all bone cuts, but before it was time to cement the components.
For optimal component sizing and positioning, a conventional preoperative templating on long and short standard radiographs was done using software in the PACS (Sectra, Linköping, Sweden). We aimed at achieving neutral mechanical axis, i.e., a hip–knee axis (HKA) of 180°.
3 doses of intravenous flucloxacillin were given within the first 8 hours, starting preoperatively, and low-molecularweight heparin was used as thromboembolic prophylaxis.
The bone preparations and instrumentation followed the Persona surgical technique manual. If necessary, ligament balancing was utilized to achieve optimal extension/flexion balance, but keeping the PCL intact. No patellar resurfacing was performed, only trimming of the bone edges, and no tourniquet was used. After routine lavage, vacuum-mixed bone cement (Palacos R+G, Heraeus, Hanau, Germany) was applied, on both the bone surfaces and components. Before closing, each patient was given local infiltration analgesia (Röstlund and Kehlet 2007).
6 to 9 tantalum markers (diameter: 0.8 mm) were positioned in both the distal femur and the proximal tibia, either diagonally through the saw cut or through the cortex (Figure 1).

Figure 1. Persona knee with femoral- and tibial tantalum markers. Cage markers are highlighted with circles.
A maximum spread of the markers in every direction of the bone was aimed for. We analyzed all RSA data with the RSAcore Model-based RSA 4.1 (MBRSA) software (RSAcore, Leiden, The Netherlands). The implant manufacturer provided the CAD models.
The reference RSA examination was performed on the 1st postoperative day. All patients had been weight-bearing, but had not started the mobilization program. Following RSA examinations were done at 3 months, and 1 and 2 years. The RSA setup was according to the standard procedure with the knee supine inside a biplanar reference cage (Tilly Medical, Lund, Sweden), with 2 simultaneously exposed digital radiographs. Translational movements are presented in mm and rotations in degrees (°). We analyzed migration along the 3 axes in an orthogonal coordinate system: x, y, and z. The results are recalculated and presented as if all knees were right-sided. Thus, positive directions for translations are medial, superior, and anterior translation along the x-, y-, and z-axes respectively. Positive directions for rotations are anterior tilt (x-axis), internal rotation (y-axis), and varus for femoral and valgus for tibial component positioning (z-axis).
For evaluation of precision of the RSA examinations, double examinations were done on at least 1 of each patient’s follow-up examinations.
The condition number indicates how well spread in the bone the tantalum markers are, and we accepted values < 120. Mean error of rigid body fitting describes stability of the markers between examinations, and we accepted values < 0.35 (Valstar et al. 2005).
Before surgery all patients were asked to fill in 2 outcome questionnaires: the Knee Injury and Osteoarthritis Outcome Score (KOOS) (Roos et al. 1998) and the Forgotten Joint Score (FJS) (Behrend et al. 2012). The same questionnaires were collected at 1 and 2 years postoperatively. The forms were posted to all patients. If there was no reply, 1 letter of reminder followed.
Statistics
With 30 patients in each group, and known data from the literature as regards standard deviations, the study was designed to have a power of at least 90% in detecting a minimal relevant difference of 0.5 mm in MTPM at year 2, having alpha = 0.05. This should also cover some dropouts.
Normality of data distribution was assessed using histograms. We used parametric tests, including Student’s t-test, for RSA data. Mean RSA values are reported with 95% confidence intervals (CI).
Visual analysis of the RSA data indicated that the majority of migration occurred up to 3 months and then levelled out. Considering this, migration over time was analyzed using a piecewise linear mixed-effect model (Qinlei Huang 2015) with a knot (breaking point) at 3 months after surgery. The models included 3 main fixed effects: group, time starting from surgery, and time starting from 3 months after surgery, and 2 interaction terms between group and the time variables. Subject was included as a random effect. These models gave the opportunity to compare the migration slopes before and after the breaking point between the 2 groups. Adjustments were made for age, sex, BMI, and ASA. Degrees of freedom was calculated based on the Kenward Roger method and an autoregressive covariance structure was used.
For PROM data evaluation, we applied non-parametric tests, including a Mann–Whitney U test and Wilcoxon signed-rank test for between-group and paired comparisons, respectively.
Statistical analyses were performed using the IBM SPSS Statistics version 26 (IBM Corp, Armonk, NY, USA) and SAS Enterprise Guide 8.1 for Windows (SAS Institute, Cary, NC, USA). A p-value of < 0.05 was considered significant.
Ethics, registration, data sharing, funding, and potential conflicts of interest
The study was approved by the Regional Ethical Board at Lund University (Dnr 2017/73), as well as the local radiation committee. The study was carried out in compliance with the Helsinki Declaration and reported according to the CONSORT guidelines. Written informed consent was received from patients before inclusion. It is registered in ClinicalTrials.gov (NCT03494348). Data is available on reasonable request.
Zimmer Biomet financially sponsored part of the RSA examinations. The authors have no conflicts of interest related to this study.
Results
RSA
27 femurs and tibias, some in different patients in the cohort, were available for analysis in each group at the 2-year RSA follow-up (Figure 2).
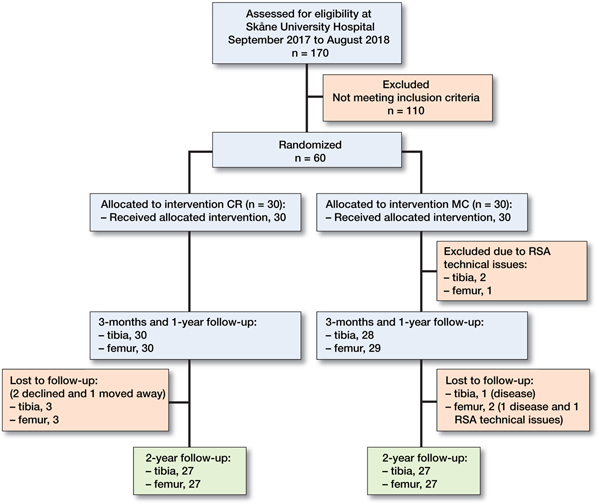
Figure 2. CONSORT Flow diagram.
There was no statistically significant difference in migration between groups at any time point for any of the measured translations, rotations, or MTPM (Figure 3 and Table 3). The mean tibial component MTPM at 2 years were 0.62 mm (CI 0.50–0.73) for the CR and 0.73 mm (CI 0.49–0.96) for the MC implant. Corresponding mean MTPM results for the femoral component at 2 years were 0.73 mm (CI 0.51–0.95) for CR and 0.58 mm (CI 0.45–0.71) for MC.

Figure 3. MTPM migration for the tibial and femoral component. Tibial figure with patient #47 both included (solid blue line) and excluded (dotted blue line)
| Segment | Implant | 3 months Mean (CI) | 1 year Mean (CI) | 2 years Mean (CI) | p–value a | |
| 0–3 m | 3–24 m | |||||
| Tibia | ||||||
| X–translation (mm) | CR | −0.01 (−0.05 to 0.03) | −0.01 (−0.05 to 0.03) | 0.02 (−0.04 to 0.07) | 0.6 | 0.9 |
| MC | −0.03 (−0.05 to −0.01) | −0.02 (−0.05 to 0.01) | −0.01 (−0.05 to 0.04) | |||
| Y–translation (mm) | CR | 0.00 (−0.03 to 0.02) | 0.01 (−0.03 to 0.05) | 0.01 (−0.03 to 0.05) | 0.5 | 0.4 |
| MC | −0.02 (−0.05 to 0.02) | −0.03 (−0.09 to 0.02) | −0.03 (−0.09 to 0.04) | |||
| Z–translation (mm) | CR | 0.00 (−0.07 to 0.06) | −0.04 (−0.11 to 0.03) | −0.01 (−0.07 to 0.06) | 0.5 | 0.8 |
| MC | −0.03 (−0.07 to 0.00) | −0.06 (−0.12 to −0.01) | −0.05 (−0.10 to 0.01) | |||
| X–rotation (°) | CR | 0.06 (−0.03 to 0.14) | 0.05 (−0.05 to 0.15) | 0.06 (−0.04 to 0.16) | 0.8 | 0.08 |
| MC | 0.04 (−0.06 to 0.14) | −0.08 (−0.36 to 0.20) | −0.16 (−0.55 to 0.23) | |||
| Y–rotation (°) | CR | −0.13 (−0.34 to 0.07) | −0.09 (−0.33 to 0.14) | −0.21 (−0.47 to 0.04) | 0.7 | 0.7 |
| MC | −0.08 (−0.36 to 0.19) | 0.03 (−0.21 to 0.26) | −0.10 (−0.39 to 0.19) | |||
| Z–rotation (°) | CR | −0.02 (−0.09 to 0.05) | 0.00 (−0.08 to 0.08) | −0.04 (−0.14 to 0.05) | 0.06 | 0.9 |
| MC | 0.04 (−0.01 to 0.08) | 0.03 (−0.03 to 0.10) | 0.02 (−0.05 to 0.09) | |||
| MTPM (mm) | CR | 0.48 (0.37 to 0.58) | 0.59 (0.48 to 0.70) | 0.62 (0.50 to 0.73) | 0.5 | 0.9 |
| MC | 0.56 (0.45 to 0.67) | 0.61 (0.45 to 0.78) | 0.73 (0.49 to 0.96) | |||
| Femur | ||||||
| X–translation (mm) | CR | −0.06 (−0.12 to −0.01) | −0.05 (−0.11 to 0.01) | −0.07 (−0.15 to 0.02) | 0.07 | 0.7 |
| MC | 0.00 (−0.04 to 0.05) | 0.00 (−0.06 to 0.05) | −0.02 (−0.09 to 0.04) | |||
| Y–translation (mm) | CR | 0.03 (−0.04 to 0.09) | 0.06 (−0.01 to 0.13) | 0.05 (−0.03 to 0.13) | 0.2 | 0.3 |
| MC | 0.00 (−0.03 to 0.02) | −0.01 (−0.05 to 0.03) | 0.00 (−0.07 to 0.06) | |||
| Z–translation (mm) | CR | 0.01 (−0.04 to 0.07) | −0.03 (−0.11 to 0.06) | −0.04 (−0.16 to 0.08) | 0.4 | 0.1 |
| MC | 0.05 (−0.02 to 0.11) | 0.06 (−0.01 to 0.13) | 0.08 (0.00 to 0.16) | |||
| X–rotation (°) | CR | 0.13 (0.05 to 0.21) | 0.20 (0.08 to 0.32) | 0.26 (0.11 to 0.41) | 0.9 | 0.7 |
| MC | 0.14 (0.04 to 0.24) | 0.20 (0.09 to 0.30) | 0.22 (0.10 to 0.35) | |||
| Y–rotation (°) | CR | 0.06 (−0.01 to 0.13) | 0.08 (−0.03 to 0.20) | 0.09 (−0.04 to 0.21) | 0.4 | 0.8 |
| MC | 0.02 (−0.07 to 0.10) | 0.05 (−0.05 to 0.15) | 0.04 (−0.08 to 0.16) | |||
| Z–rotation (°) | CR | 0.01 (−0.13 to 0.15) | 0.03 (−0.13 to 0.18) | 0.03 (−0.17 to 0.24) | 1 | 0.9 |
| MC | 0.01 (−0.06 −0.08) | 0.04 (−0.05 to 0.14) | 0.04 (−0.09 to 0.16) | |||
| MTPM (mm) | CR | 0.45 (0.31 to 0.60) | 0.62 (0.45 to 0.79) | 0.73 (0.51 to 0.95) | 0.4 | 0.4 |
| MC | 0.40 (0.31 to 0.50) | 0.51 (0.41 to 0.60) | 0.58 (0.45 to 0.71) | |||
| MTPM: maximal total point motion. CR: cruciate retaining. MC: medial congruent. CI: 95% confidence interval. a P–values from linear mixed–effect model. Slopes 0–3 months and 3–24 months. Adjusted for age, sex, BMI, and ASA. |
||||||
2 years postoperatively, the mean tibial y-translation was 0.01 mm (CI -0.03–0.05) for CR and –0.03 mm (CI –0.09 to 0.04) for the MC implant. The mean tibial x-rotation was 0.06° (CI –0.04 to 0.16) and –0.16° (CI –0.55 to 0.23) respectively at 2 years.
For the femoral component. both CR and MC had positive x-rotations 2 years after surgery with mean values of 0.26° (CI 0.11–0.41) and 0.22° (CI 0.10–0.35) respectively.
Using adjusted mixed-effect model analysis there were no statistically significant differences between groups either before 3 months or between 3 months and 2 years for any of the migration outcomes (Table 3).
1 patient (#47) in the MC group diverged considerably in tibial migration without a stabilization phase (Figure 3). The MTPM after 2 years was 3.10 mm, x-rotation -4.86°, and showed signs of radiolucency at the 2-year postoperative radiographs (Figure 4). It turned out that this patient had been included despite having a BMI above inclusion criteria and continued to gain weight during follow-up. Excluding this patient from the statistical analysis did not result in any change in significance.

Figure 4. RSA radiograph 2-year postoperative of patient #47. Arrow pointing at area of radiolucent line. The RSA show progressive backward tilt of 5°.
In the CR group, 1 patient showed large migration of the femoral component up to 3 months (MTPM 2.28 mm) but thereafter stabilized (MTPM 2 years: 2.51 mm) and we could not observe any radiographic signs of loosening.
Based on the results from double examinations, the precision in tibial x-rotation (calculated as 2SD) was 0.20° and y-translation was 0.07 mm (Table 4). There was an overall good distribution of markers with a mean condition number (SD) for tibia 22.7 (11.2) and femur 32.6 (19.5). The markers were stable over time with a mean error of rigid body fitting of 0.16 (0.08) and 0.18 (0.10) for tibia and femur, respectively. Data on the condition number and mean error was collected from the entire study population and all timepoints.
PROMs
The response rate for FJS and KOOS was between 87% and 100% in each group at the different time points.
The FJS score showed expected improvement after surgery for both groups. In the CR group, mean preoperative score was 13 and mean 2-year postoperative score was 61. The MC group improved from 11 to 60 (Figure 5).

Figure 5. Forgotten joint score (FJS). Scale 0–100, higher scores correlate with a better outcome.
In all 5 KOOS dimensions, both groups improved after the operation. There was no statistically significant difference between the CR and MC insert in any of the dimensions at any time point (Figure 6).

Figure 6. KOOS dimension scores. Scale 0–100, higher scores correlate with a better outcome.
None of the patients has so far undergone revision or had any major adverse event related to surgery, such as deep infection or pulmonary emboli.
Discussion
Our aim was to evaluate the tibial and femoral components of the Persona TKA, and especially to compare the 3D-migration behavior between 2 tibial inserts with different constraint, CR and MC. We conclude that both tibial designs stabilize as expected, without statistically significant differences between groups, in a benign migratory pattern after an initial small settling phase (Figure 3). Furthermore, the mean overall tibial migration (MTPM) of our study population appears to be in line with most previous studies on different well-performing TKA designs (Molt and Toksvig-Larsen 2014, Molt et al. 2016, Gudnason et al. 2017, Pijls et al. 2018). Even though RSA studies of the femoral implant are sparse, those existing seem to show similar results to ours (Henricson et al. 2019, Teeter et al. 2019).
At present, most TKA studies report their RSA migration values as maximal total point motion (MTPM) (Pijls et al. 2012, 2018). The MTPM is a 3D vector, referring to the point at every examination that has the maximum movement in relation to the bony reference segment. The point of maximum motion can thus be different at different examination times but indicates the overall migration over time (Valstar et al. 2005). MTPM does not specify the direction of the vector in space. We have also included the underlying individual translation and rotation results, whose significance has been pointed out previously (Gudnason et al. 2017). In a meta-analysis of 2,470 total knee arthroplasties, Pijls et al. (2018) have presented important threshold values to determine patients at risk of tibial loosening, and concluded that prosthesis migration, as measured with MTPM, of more than 0.5 mm at 6 months to be at risk and 1.6 mm to be unacceptable. After the early migration phase, the movement should be < 0.2 mm between 6 months–1 year and 1–2 years. Regarding early migration, it is important to consider the time point for the reference examination (Ornstein et al. 2000, Valstar et al. 2005). It is during the 1st months, and maybe during the 1st weeks, that a large proportion of the migration occurs. It is thus difficult to compare the actual migration value of a study where the reference examination was performed on the 1st postoperative day to another where it was performed within 1 to 2 weeks. Many studies do not even reveal the timing of the reference examination, which may lead to a bias when comparing study results. We performed the reference examination on the 1st postoperative day and our migration values thus reflect the true full migration.
Theoretically, the increased constraint on the medial side of the MC insert, compared with CR, could have affected the migration pattern, due to a plausible asymmetric load on the inlay. However, unlike some other pivoted TKAs on the market, the MC Persona knee system is not a purely “ball-in-socket” restricted TKA, which relies on a single radius curvature in symmetrical femoral condyles and a spherical and fully congruent medial compartment. Instead, the Persona knee has a J-curved femoral design with asymmetric posterior sagittal radii and an anatomical tibial baseplate, fitted with either an MC or CR polyethene insert. Thus, in this study we compare 2 different polyethylene inserts, and with the exception of a slight tendency toward an anterior tilt of the femoral component, seen in both groups, there was no clear pattern of translation or rotation for either the tibial or femoral components, and the migration values were small (Table 3).
1 patient in the MC group (patient #47) showed a deviating tibial migration pattern. Already at 3 months, this patient had a tibial backward tilt (x-rotation) of –0.9°, in comparison with a slight forward tilt of 0.1° for the other patients in the MC group. At 2 years, the tibial backward tilt was almost 5° and showed clear signs of loosening on standard radiographs (Figure 4). Rotation around the transverse axis, as well as proximal and distal translation, has been shown by Gudnason et al. (2017) to be better at predicting aseptic loosening than MTPM. In retrospect, this patient should not have been included due to a BMI of 40 at time of surgery, which is well above the inclusion level of 35. Furthermore, the patient continued to gain weight during follow-up. We chose to keep the patient in the study and the case is interesting to describe separately. The high BMI and also a quite severe preoperative varus deformity of 13° are risk factors (Ritter et al. 2013, Roche et al. 2018) and may have contributed to the migration pattern. No disturbing knee symptoms have so far been reported, and PROMs are similar to the overall mean. We do, however, foresee that this patient’s tibial component will need later revision. Excluding this patient retrospectively would not have changed the statistical significance of the results but changes the appearance of the graphs as shown in Figure 3. We believe this case underscores the ability of RSA to early on predict later loosening.
Our results for KOOS were in line with previous studies on the Persona TKA with a different kind of constraints (PS, CR, and UC) (Galea et al. 2019, Mathijssen et al. 2019).
The FJS appears to solve some of the problems with ceiling effects, i.e., the ability to distinguish between patients with good and excellent outcomes (Behrend et al. 2012). In a recent meta-analysis, the medially stabilized TKAs scored higher versus non-medially stabilized TKAs, although just below the minimal clinically important difference of 14 points for FJS (Tso et al. 2021). Hasan et al. (2020) found similar FJS results to ours, without any difference between cemented and cementless CR TKAs. French et al. (2020) compared the Vanguard Cruciate-Retaining Knee with a medially stabilized SAIPH Knee and concluded that the medially stabilized knee scored better on the FJS as well as the quality-of-life KOOS subscale. We were unable to show any difference in PROMs between the CR and MC group, keeping in mind, however, that our study was not powered for PROMs evaluation but for RSA.
With the MC being the most recent type introduced to the market, the 1st mid- to long-term studies have been published. In a study on the ADVANCE Medial Pivot knee, a survival analysis showed a cumulative success rate of 98.8% at 17 years (Macheras et al. 2017) and a meta-analysis on medial pivot implants demonstrated a pooled component survivorship estimate to be 97.6% (95% CI 95.8–98.6) after 8 years (Fitch et al. 2014).
A TKA aligned to the mechanical axis of the lower limb in the coronal plane has been the gold standard for many years (Schiraldi et al. 2016) and was also what we aimed to achieve. Howell et al. (2008) described the kinematic alignment method to restore the constitutional knee joint by creating bone resections parallel to the pre-disease surface of the distal femur and proximal tibia, as opposed to a straight-line mechanical axis. Studies on kinematic alignment have shown promising results, both for the Persona TKA with MC insert, as well as other TKA designs (Courtney and Lee 2017, Risitano et al. 2020). With this said, it is still under debate whether the alignment is a question on which you need to compromise between patient satisfaction and implant survivorship, as the mechanically aligned TKA might benefit the latter. It would have been interesting to see if our results had been different if we aimed for kinematical instead of mechanical alignment.
A possible limitation of this study is the number of patients and the short follow-up. For an RSA study, 60 patients are sufficient and 2 years’ follow-up is normally enough, but for an adequate assessment of PROM data a larger cohort would have been needed. Another limitation is the fact that, to avoid the issue of multiplicity, we based our power calculation on MTPM, and not on individual axes translation and rotation, even though this was stated to be our primary endpoint in the trial registration.
Conclusion
Our RSA results for the cemented Persona TKA demonstrate good migratory patterns for both the femoral and tibial components, fully in line with other well-performing total knee replacements on the market. Furthermore, we could not show any statistically significant difference regarding either migration or PROMs between the MC or CR inlays up to 2 years.
Behrend H, Giesinger K, Giesinger J M, Kuster M S. The “forgotten joint” as the ultimate goal in joint arthroplasty: validation of a new patient-reported outcome measure. J Arthroplasty 2012; 27(3): 430-6.e1. doi: 10.1016/j.arth.2011.06.035.
Blaha J D. The rationale for a total knee implant that confers anteroposterior stability throughout range of motion. J Arthroplasty 2004; 19(4 Suppl. 1): 22-6. doi: 10.1016/j.arth.2004.04.002.
Bourne R B, Chesworth B M, Davis A M, Mahomed N N, Charron K D. Patient satisfaction after total knee arthroplasty: who is satisfied and who is not? Clin Orthop Relat Res 2010; 468(1): 57-63. doi: 10.1007/s11999-009-1119-9.
Cassar-Gheiti A J, Jamieson P S, Radi M, Wolfstadt J I, Backstein D J. Evaluation of the medial stabilized knee design using data from national joint registries and current literature. J Arthroplasty 2020; 35(7): 1950-5. doi: 10.1016/j.arth.2020.02.026.
Courtney P M, Lee G C. Early outcomes of kinematic alignment in primary total knee arthroplasty: a meta-analysis of the literature. J Arthroplasty 2017; 32(6): 2028-32.e1. doi: 10.1016/j.arth.2017.02.041.
Fitch D A, Sedacki K, Yang Y. Mid- to long-term outcomes of a medial pivot system for primary total knee replacement: a systematic review and meta-analysis. Bone Joint Res 2014; 3(10): 297-304. doi: 10.1302/2046-3758.310.2000290.
French S R, Munir S, Brighton R. A single surgeon series comparing the outcomes of a cruciate retaining and medially stabilized total knee arthroplasty using kinematic alignment principles. J Arthroplasty 2020; 35(2): 422-8. doi: 10.1016/j.arth.2019.09.021.
Galea V P, Botros M A, Madanat R, Nielsen C S, Bragdon C. Promising early outcomes of a novel anatomic knee system. Knee Surg Sports Traumatol Arthrosc 2019; 27(4): 1067-74. doi: 10.1007/s00167-018-5248-0.
Gudnason A, Adalberth G, Nilsson K G, Hailer N P. Tibial component rotation around the transverse axis measured by radiostereometry predicts aseptic loosening better than maximal total point motion. Acta Orthop 2017; 88(3): 282-7. doi: 10.1080/17453674.2017.1297001.
Hasan S, van Hamersveld K T, Marang-van de Mheen P J, Kaptein B L, Nelissen R, Toksvig-Larsen S. Migration of a novel 3D-printed cementless versus a cemented total knee arthroplasty: two-year results of a randomized controlled trial using radiostereometric analysis. Bone Joint J 2020; 102-b(8): 1016-24. doi: 10.1302/0301-620x.102b8.Bjj-2020-0054.R1.
Henricson A, Wojtowicz R, Nilsson K G, Crnalic S. Uncemented or cemented femoral components work equally well in total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 2019; 27(4): 1251-8. doi: 10.1007/s00167-018-5227-5.
Howell S M, Kuznik K, Hull M L, Siston R A. Results of an initial experience with custom-fit positioning total knee arthroplasty in a series of 48 patients. Orthopedics 2008; 31(9): 857-63. doi: 10.3928/01477447-20080901-15.
Kärrholm J, Borssén B, Löwenhielm G, Snorrason F. Does early micromotion of femoral stem prostheses matter? 4-7-year stereoradiographic follow-up of 84 cemented prostheses. J Bone Joint Surg Br 1994; 76(6): 912-7.
Kärrholm J, Saari T. Removal or retention—will we ever know? The posterior cruciate ligament in total knee replacement. Acta Orthop 2005; 76(6): 754-6. doi: 10.1080/17453670510045336.
Macheras G A, Galanakos S P, Lepetsos P, Anastasopoulos P P, Papadakis S A. A long term clinical outcome of the Medial Pivot Knee Arthroplasty System. Knee 2017; 24(2): 447-53. doi: 10.1016/j.knee.2017.01.008.
Malchau H, Bragdon C R, Muratoglu O K. The stepwise introduction of innovation into orthopedic surgery: the next level of dilemmas. J Arthroplasty 2011; 26(6): 825-31. doi: 10.1016/j.arth.2010.08.007.
Mathijssen N M C, Verburg H, London N J, Landsiedl M, Dominkus M. Patient reported outcomes and implant survivorship after total knee arthroplasty with the Persona knee implant system: two year follow up. BMC Musculoskelet Disord 2019; 20(1): 97. doi: 10.1186/s12891-0192470-y.
Molt M, Toksvig-Larsen S. Similar early migration when comparing CR and PS in Triathlon™ TKA: a prospective randomised RSA trial. Knee 2014; 21(5): 949-54. doi: 10.1016/j.knee.2014.05.012.
Molt M, Ryd L, Toksvig-Larsen S. A randomized RSA study concentrating especially on continuous migration. Acta Orthop 2016; 87(3): 262-7. doi: 10.3109/17453674.2016.1166876.
Ornstein E, Franzén H, Johnsson R, Sundberg M. Radiostereometric analysis in hip revision surgery—optimal time for index examination: 6 patients revised with impacted allografts and cement followed weekly for 6 weeks. Acta Orthop Scand 2000; 71(4): 360-4. doi: 10.1080/000164700317393349.
Pijls B G, Valstar E R, Nouta K A, Plevier J W, Fiocco M, Middeldorp S, Nelissen R G. Early migration of tibial components is associated with late revision: a systematic review and meta-analysis of 21,000 knee arthroplasties. Acta Orthop 2012; 83(6): 614-24. doi: 10.3109/17453674.2012.747052.
Pijls B G, Plevier JWM, Nelissen R. RSAmigration of total knee replacements. Acta Orthop 2018; 89(3): 320-8. doi: 10.1080/17453674.2018.1443635.
Qinlei Huang. Hands-on tutorial for piecewise linear mixed-effects models using SAS® PROC MIXED (Ed St Jude Children’s Research Hospital M, TN). PharmaSUG China 2015-08; 2015.
Risitano S, Sabatini L, Barberis L, Fusini F, Malavolta M, Indelli P F. Combining kinematic alignment and medial stabilized design in total knee arthroplasty: basic rationale and preliminary clinical evidences. J Orthop 2020; 21: 427-31. doi: 10.1016/j.jor.2020.08.025.
Ritter M A, Davis K E, Davis P, Farris A, Malinzak R A, Berend M E, Meding J B. Preoperative malalignment increases risk of failure after total knee arthroplasty. J Bone Joint Surg Am 2013; 95(2): 126-31. doi: 10.2106/jbjs.K.00607.
Roche M, Law T Y, Kurowicki J, Rosas S, Rush A J, 3rd. Effect of obesity on total knee arthroplasty: costs and revision rate. J Knee Surg 2018; 31(1): 38-42. doi: 10.1055/s-0037-1608933.
Roos E M, Roos H P, Ekdahl C, Lohmander L S. Knee injury and Osteoarthritis Outcome Score (KOOS): validation of a Swedish version. Scand J Med Sci Sports 1998; 8(6): 439-48. doi: 10.1111/j.1600-0838.1998.tb00465.x.
Ryd L, Albrektsson B E, Carlsson L, Dansgård F, Herberts P, Lindstrand A, et al. Roentgen stereophotogrammetric analysis as a predictor of mechanical loosening of knee prostheses. J Bone Joint Surg Br 1995; 77(3): 377-83.
Röstlund T, Kehlet H. High-dose local infiltration analgesia after hip and knee replacement: what is it, why does it work, and what are the future challenges? Acta Orthop 2007; 78(2): 159-61. doi: 10.1080/17453670710013627.
Schiraldi M, Bonzanini G, Chirillo D, de Tullio V. Mechanical and kinematic alignment in total knee arthroplasty. Ann Transl Med 2016; 4(7): 130. doi: 10.21037/atm.2016.03.31.
Teeter M G, Marsh J D, Howard J L, Yuan X, Vasarhelyi E M, McCalden R W, Naudie D D R. A randomized controlled trial investigating the value of patient-specific instrumentation for total knee arthroplasty in the Canadian healthcare system. Bone Joint J 2019; 101-b(5): 565-72. doi: 10.1302/0301-620x.101b5.Bjj-2018-1323.R1.
Tso R, Smith J, Doma K, Grant A, McEwen P. Clinical and patient-reported outcomes of medial stabilized versus non-medial stabilized prostheses in total knee arthroplasty: a systematic review and meta-analysis. J Arthroplasty 2021; 36(2): 767-76.e2. doi: 10.1016/j.arth.2020.07.086.
Valstar E R, Gill R, Ryd L, Flivik G, Börlin N, Kärrholm J. Guidelines for standardization of radiostereometry (RSA) of implants. Acta Orthop 2005; 76(4): 563-72. doi: 10.1080/17453670510041574.